What people does scid affect more4/4/2024 
We have reported here the longest follow-up of a post-transplant SCID patient who, to our knowledge, bears the first gamma chain (γc) variant to show intact IL-21 signaling.Ĭase Presentation: The patient presented at 5 months of age with recurrent thrush and Pneumocystis jiroveci pneumonia. There is a growing number of post-transplant SCID patients, and it is imperative to assess the long-term outcomes of these patients. First performed in the late 1960's, hematopoietic stem cell transplantation remains the standard treatment for most cases of SCID. Introduction: Severe Combined Immunodeficiency (SCID) is a life-threatening immunodeficiency caused by several pathogenic genetic variants, and it is characterized by profound defects in T-cell numbers and immune function. Division of Immunology, Allergy, and Rheumatology, Department of Pediatrics, University of California, Los Angeles, Los Angeles, CA, United States.SCID should be considered a pediatric emergency.Christin Deal † Timothy J. 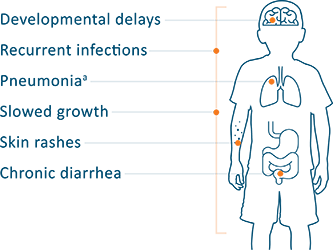
She goes on to say, “…essentially every baby with SCID coud be cured if diagnosed early enough. If found later, less effective treatment can run into the millions. A simple blood test could allow us to treat, and most likely cure, SCID in an infant at a reasonable cost. Such a blood test could pick up children with SCID as well as those with other serious immune deficiencies that would not be apparent until the child developed an infection. Rebecca Buckley, Chief of Duke University’s Division of Pediatric Allergy and Immunology, “Early diagnosis of SCID is rare because doctors do not routinely perform a blood test on newborns to count white blood cells. As a result, the immune system of the afflicted individual is severely compromised or completely lacking.Īccording to Dr. Immature lymphoid cells of the immune system are particularly sensitive to the toxic effects of these unused substrates, so fail to reach maturity. 
This means that the substrates for this enzyme accumulate in cells. In another form of SCID, there is a lack of the enzyme adenosine deaminase (ADA), coded for by a gene on chromosome 20. Defective receptor pathways prevent the proper development of T-lymphocytes, cells that play a key role in identifying invading agents and activating other cells of the immune system. A mutation in JAK3, located on chromosome 19, can also result in SCID. Though invasive, new treatments such as bone marrow and stem-cell transplantation save as many as 80% of SCID patients.Īll forms of SCID are inherited, with as many as half of SCID cases linked to the X chromosome, passed on by the mother. Without a functional immune system, SCID patients are susceptible to recurrent infections and may die before the first year of life. The defining feature of SCID, commonly called “bubble boy” disease, is a defect in the specialized white blood cells (B- and T-lymphocytes) that defend us from infection by viruses, bacteria and fungi. SCID, or “bubble boy disease,” became a household name during the 1970’s with the filming of David Vetter, a boy who lived for 12 years in a plastic, germ-free bubble. They may include pneumonia, meningitis or bloodstream infections. Severe combined immunodeficiency (SCID) represents a group of rare, sometimes fatal, primary immunodeficiencies characterized by one or more serious, life-threatening infections within the first few months of life. Secondary immune deficiencies can be caused by exposure to radiation or toxic chemicals, chemotherapy, malnutrition and burns. When the damage is caused by an environmental agent, the resulting disease is referred to as secondary immune deficiency disease. Primary immune deficiency disease affect many thousands of children and adults in the U.S. According to the World Health Organization, there are more than 200 of these sometimes life-altering or life-threatening inherited defects – some are relatively rare, some are quite common. In the case of an inherited defect, the resulting disease is referred to as primary immune deficiency disease. An immune deficiency disease may be caused either by an inherited defect in the cells of the immune system or by an environmental agent.
0 Comments
Leave a Reply.AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
